An elderly patient with history of treatment for ulcerative colitis for over 2 decades presented to emergency with acute intestinal obstruction. Contrast enhanced abdominal CT scan was suggestive of large bowel obstruction with stricture in proximal sigmoid colon. The patient underwent sigmoidoscopy with self-expanding metallic stent (SEMS) placement as bridge to elective surgery. The biopsy was suggestive of adenocarcinoma in the background of ulcerative colitis (UC). Further oncology work up including whole body PET scan did not reveal any metastatic disease. Two weeks later, laparoscopy assisted total proctocolectomy with ileal pouch anal anastomosis was performed. The postoperative period was uncomplicated and the patient was discharged on 7th postoperative day. The biopsy revealed moderately differentiated adenocarcinoma T3N0 (> 20 regional lymph nodes examined) in the background of ulcerative colitis. All surgical margins were clear (Figure 1).
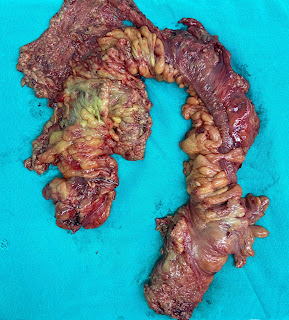
Figure1. Proctocolectomy specimen
This case highlights the importance of regular follow up (including surveillance colonoscopy) for patients with ulcerative colitis.
SEMS are increasingly utilized in malignant left colonic obstructions as bridge to elective surgery. A recent meta-analysis of 33 studies involving 15224 patients compared the outcomes of emergency resection, diverting stoma and SEMS placement for obstructing left colon cancer.1 A bridging interval of 02 weeks following SEMS placement has been reported as appropriate.2
A recent systematic review and meta-analysis (25 studies) compared the survival outcomes of inflammatory bowel disease (IBD) associated (8034 patients) and non IBD associated (810526 patients) colorectal cancer (CRC). Cancer specific survival for IBD – CRC was poorer than those without IBD. Of the IBD – CRC patients, UC patients had favorable overall survival when compared to Crohn’s disease patients. The IBD associated CRC was characterized by increased rate of unfavorable histologic features such as poor differentiation and signet ring carcinoma, right sided tumors and reduced rate of R0 resections.3
Development of colorectal cancer is one of the most serious complication of ulcerative colitis. Cumulative risk of development of cancer reaches 25% at 25 years, rising up to 65% at 40 years of disease duration. Patients with involvement of entire colon have increased risk as compared to those with disease confined to the left side of the colon. A surveillance colonoscopy is recommended every 1-2 years beginning 8 years after pancolitis and 12-15 years after the onset of left sided colitis.4
References
1. Jain SR, Yaow C Y L, Ng CH. Comparison of colonic stents, stomas and resection for obstructive left colon cancer: a meta-analysis. Tech Coloproctol 2020;24(11); 1121-1136
2. Velde J V, Kumcu A, Amlung F J et al. Time interval between self-expandable metal stent placement or creation of a decompressing stoma and elective resection of left-sided obstructive colon cancer Endoscopy 2021; 53(9):905 -13
3. Can Lu, Josefine S, Zhang T et al. Survival outcomes and clinicopathological features in inflammatory bowel disease associated colorectal cancer. A systematic review and meta- analysis. Ann Surg 2022;276(5):e319-330
4. Townsend CM, Beauchamp RD, Evers BM, Mattox KL (2017) Sabiston textbook of surgery, first south asia edition (20th edition). Elsevier Page 1342
Authors:
Dr Nitin Vashistha, MS, FIAGES, FACS
Dr Dinesh Singhal, MS, FACS, DNB (Surg Gastro)
Department of Surgical Gastroenterology,
Max Super Speciality Hospital, Saket, New Delhi, India
E mail: gi.cancer.india@gmail.com




